The US Leader is NOW in Mexico. Procedures ONLY $3750 for 25 million stem cells!
NEW PROMO: Treatments > 50 million cells receive FREE 25 BILLION Exosomes IV!*
The US Leader is NOW in Mexico. Procedures ONLY $3750 for 25 million stem cells!
NEW PROMO: Treatments > 50 million cells receive FREE 25 BILLION Exosomes IV!*
Spinal cord injury (SCI) results from a mechanical injury to the spinal column. Worldwide, over 700,000 individuals sustain a spinal cord injury. This could be the result of a penetrating trauma (e.g. bullet) or blunt force trauma (e.g. car accident).
Eighty percent of spinal injuries occur in men, with 55% of injuries being in the cervical region. The rest are evenly split 15% each in the thoracic, thoracolumbar and lumbar. The average age of an individual sustaining an SCI is just over 40. What that means is without significant recovery, those affected will need substantial care for decades. Estimates for the economic burden of lifelong care average $4 million.
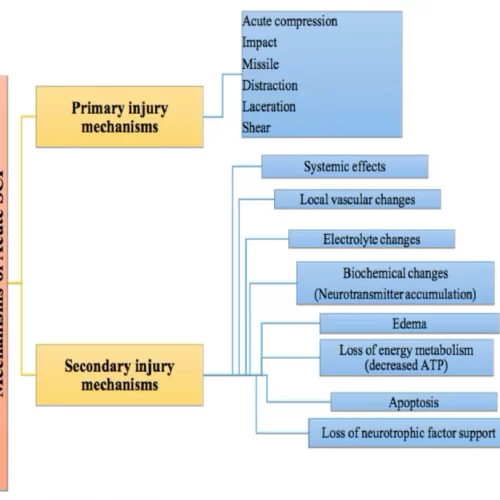
Spinal cord injury disrupts the nerve connections between the brain and the body, resulting in paralysis. There are two mechanisms of injury from an SCI, known as primary and secondary.
Primary Injury: Refers to the acute initial event. This could be any of the following:
Secondary Injury:
The secondary cascade of injury occurs in the hours and days after the initial injury.
This includes ischemia, anoxia, inflammation, swelling, cell death and scar formation.
While this is a complicated process, not much of these processes are actually helpful for healing. Free radicals accumulate, electrolye abnormalities occur, heart function decreases, blood pressure drops, and blood vessels spasm reducing blood flow.
Initial treatment includes ICU support and often high doses of steroids. Blood pressure stabilization is critical. Surgery may be needed to stabilize the spine.
There are spontaneous healing mechanisms activated, such as endogenous stem cell activation, remyelination and neural plasticity. But without some sort of exogenous assistance, they have not resulted in significant functional recovery.
The goal with using stem cells for SCI is to achieve some meaningful functional recovery with safe biologics that provide more benefit than risks. To date, the best outcomes so far have been seen with what’s termed Adult Stem Cells and not Embryonic Stem Cells.
What does this mean? Well, embryonic stem cells are the ones that come from either aborted fetuses or left over embryos after an in vitro fertilization. Using them clinically may result in a significant rejection reaction, or possibly a tumorigenic response. Therefore, they are not ready for clinical use.
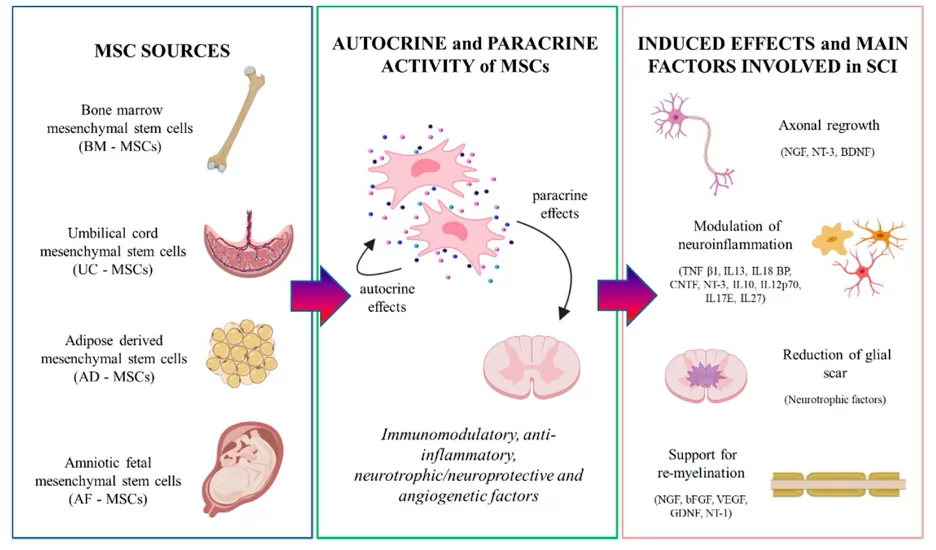
The tissue consists of the umbilical cord, amniotic fluid and placenta. As weird as it sounds, the stem cells that come from the tissue fall into the adult stem cell category. The tissue is extremely rich in mesenchymal and hematopoetic stem cells, cytokines, growth factors, exosomes, secretomes, mRNA, translational proteins and hyaluronic acid.
What are the specific goals for patients undergoing stem cell therapy for spinal cord injury?
In humans, regeneration of neurons may seem like a pipe dream. But all one needs to do is look at the salamander to see that it is possible to have proliferation of glial cells to stimulate axon growth, recreate the neural tube and regain significant function!
When looking at clinical studies on stem cells for SCI, comparisons between them can be difficult. This relates to the differences in numbers of cells used, types of cells and time differences in chronicity of SCI.
However, one overlying positive is just how safe the usage of adult stem cells has been. Most complications during studies using adult stem cells for SCI have shown minimal issues related to the stem cells themselves and more to simply the fact that the patient has a SCI and related effects.
How do injected stem cells actually help when injected directly into the spinal cord? There are various theories, one of which is that the cells indirectly affect axon regeneration. This involves activating the endogenous stem cells, removal of scarring and forming extracellular matrix to guide the regenerating axons.
Neuroprotection from MSC’s occurs due to the release of a number of neurotrophic factors. This may include brain-derived growth factor, glial derived growth factor, nerve growth factor, and basic fibroblast growth factor. The combination of these growth factors is instrumental I preventing nerve degeneration and cell death, while on the other hand supporting neurogenesis, axon growth, remyelination and cell metabolism.
In the video below, R3 CEO David Greene, MD, MBA, goes through several clinical studies looking at using MSC’s for spinal cord injury and the results.
R3 Stem Cell International Offers Amazingly Effective Regenerative Procedures For Spinal Cord Injury. Several Options Are Available, With Up To A Billion Live, Active Stem Cells!
The Process For Receiving Stem Cell Treatment For Spinal Cord Injury Starts With A Free Phone Consultation, Simply Call Us Today At +1 (888) 988-0515.
References:
Current Status and Future Strategies to Treat Spinal Cord Injury with Adult Stem Cells, Jeong et al, 2020, J Korean Neurosurg Soc, 153-162.
Mesenchymal Stem Cells for Spinal Cord Injury:
Current Options, Limitations, and Future of Cell Therapy, Cofano et al, Int Journal of Molecular Sciences, 2019. Clinical observation of umbilical cord mesenchymal stem cell transplantation in treatment for sequelae of thoracolumbar spinal cord injury, Cheng et al, J Transl Med 2014.
Indications For Stem Cell Therapy At R3 Centers:
“The Clinic And Staff Are Very Professional. I Had A Great Time, From Their Pick Up In San Diego, To My Hotel In Tijuana. The Procedure At The Clinic Is Quite Simple. In A Few Hours, Everything Is Finished. The Doctor Explained The Injections To Me (Intravenous, In The Hip, And In The Back, At My Request) And Seems To Be Passionate About Stem Cells, It Was A Pleasure To Chat With Him 🙂
I Can Encourage You To Go To This Clinic.”
Julien B, Canada
The Response To Our Mexico Stem Cell Programs Have Been OVERWHELMING!
Make Sure To Reserve Your Spot Now By Calling Us At (888) 988-0515.
Our Experienced Providers Will Perform A Free Phone Consultation To See If You Are A Candidate.
R3 Stem Cell Offers Financing Options
For North American Residents, Wherever They Obtain Procedures!


Stem Cell Doctors In Mexico
Offering Regenerative Therapies by Injection and IV starting at only $3750!
R3 Stem Cell International’s Centers of Excellence offer Cutting Edge regenerative medicine treatments with highly skilled, compassionate physicians in Tijuana and Cancun Mexico. The Mexico program involves chaperoned transportation over the border and stem cell treatments that are less than half what individuals pay in the US for more than double the stem cell counts! The treatments offered include stem cell injections, IV Therapy, Nebulizer or Intra-nasal.
R3 Stem Cell International is not offering stem cell therapy as a cure for any medical condition. No statements on this site have been evaluated or approved by the FDA.
This site contains no medical advice. All procedures with R3 Stem Cell International are performed outside the United States.






Copyright © 2016 – 2023 R3 Stem Cell